Eczema (EG-zeh-muh), also known as atopic dermatitis, is a common skin condition that affects babies and young children, often improving naturally as children grow. However, it can sometimes persist into adolescence and adulthood. Eczema symptoms typically begin before a child reaches 1 year old, and up to 25% of children are affected.
For parents, eczema often shows up as dry, itchy, or irritated skin that can be uncomfortable — and sometimes frustrating — to manage. The good news is that with the right care, most children’s symptoms can be well controlled.
The American Academy of Pediatrics (AAP) released updated guidance for managing eczema in 2025, emphasizing proactive care, mental health impacts, and emerging therapies.
Below, we answer common questions parents have about caring for a child with eczema and what these new recommendations mean for families.
What causes eczema in children?
Atopic dermatitis, also known as eczema, is a chronic, inflammatory skin condition. Eczema leads to dry, inflamed, itchy skin.
The cause of eczema is complex and due to multiple factors, including genetics, environmental triggers, and dysfunction of the skin barrier and immune system. Children with eczema often have skin barrier dysfunction, including a lack of a special protein called “filaggrin” in the outer layer of skin. Environmental factors can trigger eczema flares, such as harsh or scented skin products, abrasive clothing, and changes in environmental humidity. Additionally, parents with eczema are more likely to have children with eczema.

What are eczema symptoms in kids?
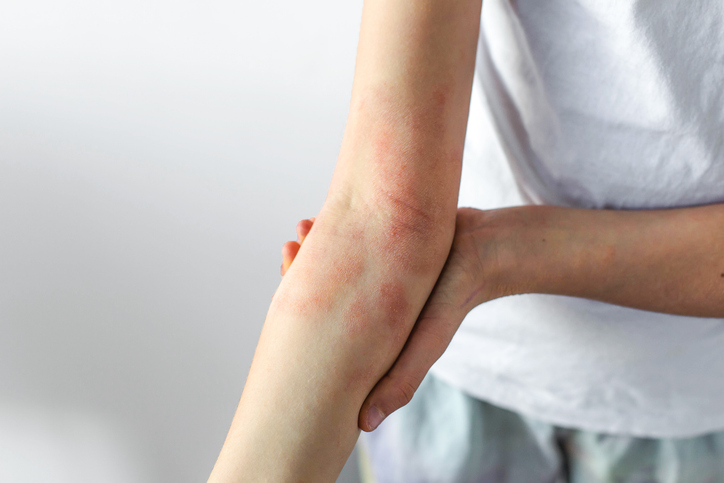
The rash of eczema can include dry skin, itchy or irritated skin, and a rash with redness and bumps. In school-aged children, the eczema rash is often in elbow creases, the backs of the knees, on the neck, and around the eyes. When parents talk about “baby eczema,” it’s common for the rash to appear on an infant’s face, especially on the cheeks, and sometimes the scalp, wrists, and ankles. The 2025 AAP clinical report noted that eczema symptoms are typically more severe in both Black and Hispanic children, and both groups are more likely to miss school because of the condition.
Will eczema go away? Is eczema contagious?
Eczema is not curable and it’s not contagious, but with proper treatment and medication, the disease can be well managed. And although there’s no cure, avoiding triggers and following a good skincare routine can greatly reduce flareups. Additionally, about half of all affected children experience improvement with their eczema between ages 5 and 15. The key is identifying your child’s specific triggers and working with a pediatrician or pediatric specialist to develop an effective management plan.
What are triggers for eczema in kids?
Eczema flareups occur when something “switches on” the immune system, causing skin cells to not behave as they should. While the exact cause isn’t fully understood, it results from a combination of genetic and environmental factors. The main triggers that can cause an eczema flare are dry skin, irritants, stress, allergies, infection, and heat or sweating. It’s important to note that these are triggers that worsen the symptoms of eczema, but are not the cause of eczema.

What are common misconceptions parents have about eczema?
Many parents believe eczema is caused by external factors such as allergens or food, but this is typically incorrect. The 2025 AAP report confirms that while up to 40% of children with eczema also have food allergies, foods do not cause the eczema itself. Foods may trigger flareups in some children with severe eczema, but they are not the underlying cause.
What’s the biggest misunderstanding families have about treating an eczema flare up?
Families often think the only change to make when treating a flare is to use topical steroid medication. However, the most important thing to do during a flare is to increase the use of moisturizers (in addition to following the flare care plan from your child’s doctor). Kids with eczema should always feel like they recently applied moisturizer. If they get dry, reapply!
What’s the 3-Minute Rule for eczema?
The 3-Minute Rule is a simple yet effective skincare technique for managing eczema in children. It involves applying a thick moisturizer within three minutes of bathing to maximize hydration and protect the skin barrier.

When do you add prescriptions versus daily routine care?
All children with eczema should have a daily moisturizing routine, which is achieved with over-the-counter moisturizing ointments, creams, and lotions. The best moisturizers are the ones that are used regularly! This means at least twice a day, if not more.
All kids should also have a plan for flares, which will typically include a topical steroid. The topical steroids offered over the counter are particularly weak in potency, so your child’s primary care pediatrician, pediatric dermatologist, or pediatric allergy and immunology specialist will likely prescribe a topical steroid for your child to help with their flares.
A new AAP report covered several emerging therapies that have become available, providing hope for families who have struggled with traditional treatment options. It recommends these therapies primarily for children with moderate to severe atopic dermatitis not adequately controlled with traditional approaches. The report also includes encouraging updates, such as dupilumab is now approved for infants as young as 6 months, and studies show improved safety and effectiveness outcomes for both new and existing therapies. Families dealing with severe eczema can learn more about these options from an eczema specialist.
When should you call the doctor for eczema treatment?
If you see signs of baby eczema, you should take your infant to see their pediatrician as soon as possible because early diagnosis and treatment is more effective. If your child is older and has been diagnosed with eczema, you’ll want to make an appointment if your child’s eczema symptoms begin affecting daily activities or causing emotional distress. This would include frequent flareups that are difficult to control, any sleep disruption, or their eczema rash is not improving with the usual treatments.
Seek immediate care if you see anything that looks like an infection, swollen areas, pus, spreading redness, or oozing scabs. Eczema infections are very treatable but they can range from mild to life-threatening, so early recognition and treatment are key to good outcomes.
The post Eczema in Kids: A Parent’s Guide to Symptoms, Triggers, and Care appeared first on Nemours Blog | Expert Guidance on Children's Health and Wellness.
